Navigating Pathways to Sustainable Addiction Recovery
Recovery from addiction and mental health challenges is a deeply personal journey. It is a path toward wellness, meaningful relationships, and a life filled with purpose. Many people face both addiction and mental health issues together. This makes the journey to healing even more complex.

We understand this challenge. This guide will help you navigate the landscape of addiction recovery and mental health. We will explore how these conditions are linked. We will also discuss effective treatments and practical strategies for lasting well-being. Our goal is to provide clear insights and actionable steps. These steps can support you or your loved ones on the path to sustainable recovery.
SAMHSA defines recovery as a process where individuals improve their health, live self-directed lives, and reach their full potential. This includes four key areas:
- Health: Managing conditions and making healthy choices.
- Home: Having a stable and safe place to live.
- Purpose: Engaging in meaningful daily activities.
- Community: Building supportive relationships.
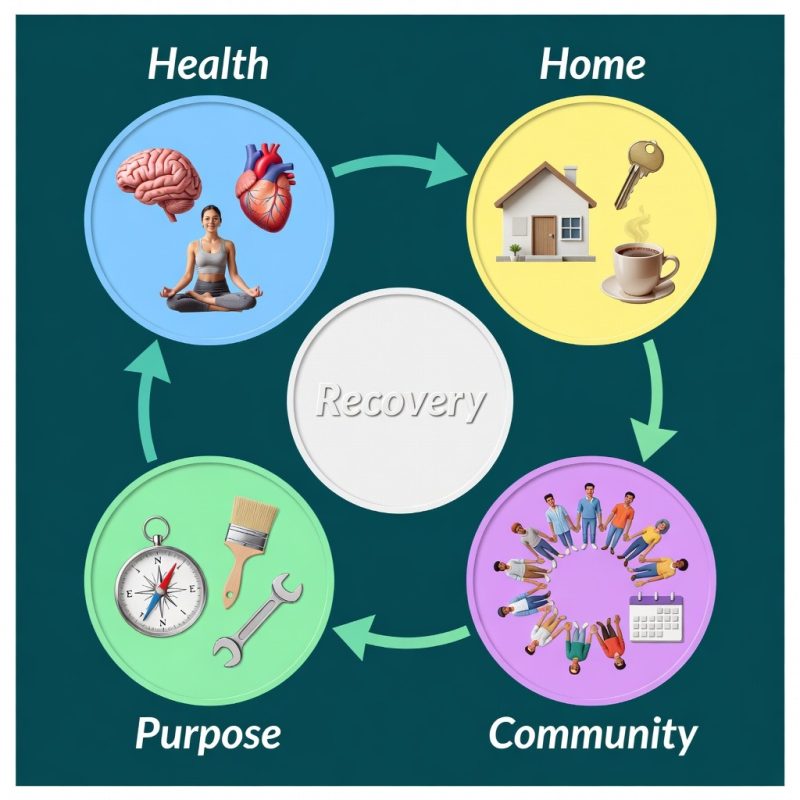
This article will break down these elements. We aim to show how integrated care can lead to a more complete and fulfilling recovery.
Verify your insurance coverage today
The relationship between addiction and mental health is intricate and often bidirectional. It’s rare for someone to experience a substance use disorder (SUD) without also facing mental health challenges, or vice versa. This complex interplay gives rise to what we call concurrent disorders or dual diagnoses. These terms describe the situation when an individual struggles with both a mental health condition and a substance use disorder simultaneously. Understanding this link is crucial for effective addiction treatment and sustainable recovery.
At the heart of this connection lies a concept known as bidirectional risk. This means that mental health conditions can increase the likelihood of developing a substance use disorder, and substance use disorders can, in turn, trigger or worsen mental health conditions. For instance, someone experiencing anxiety or depression might turn to alcohol or drugs as a form of self-medication, seeking temporary relief from distressing symptoms. While this might offer short-term comfort, it often exacerbates the underlying mental health issue in the long run, creating a vicious cycle.
Furthermore, genetic vulnerability plays a significant role. Research indicates that certain genetic predispositions can increase an individual’s susceptibility to both mental health disorders and addiction. If a family history of depression or alcoholism exists, the risk for concurrent disorders may be higher. Environmental factors, such as chronic stress, trauma, or adverse childhood experiences, also act as powerful environmental triggers that can contribute to the development of both conditions. These stressors can overwhelm an individual’s coping mechanisms, making them more vulnerable to seeking solace in substances.
Addressing these intertwined issues requires a comprehensive and integrated approach, such as the personalized addiction and mental health plans offered by SoberSteps, which recognize the unique complexities of each individual’s journey. Whether it’s navigating the challenges of drug addiction or understanding the specific impacts of stimulant addiction, a holistic perspective is key to fostering healing and long-term well-being.
The Prevalence of Co-occurring Disorders in Addiction Recovery and Mental Health
The co-occurrence of mental health and substance use disorders is remarkably common, highlighting the critical need for integrated treatment approaches. Statistics reveal the widespread nature of this challenge. For instance, a significant 72.1% of U.S. adults aged 18 and older who perceived they had ever had a substance use and/or mental health problem considered themselves to be in recovery or recovered. This translates to an impressive 50.2 million people finding their way back to health, underscoring the hope and possibility inherent in recovery.
However, the journey often involves navigating both conditions simultaneously. In a 2020 U.S. survey, 6.7% of adults, or 17.0 million people, reported having both a mental illness and a substance use disorder in the past year. This statistic alone illustrates the substantial overlap between these two health concerns.
Looking closer at specific mental health conditions, the rates of co-occurrence with substance abuse are even more striking:
- Roughly 50% of individuals with severe mental disorders are also affected by substance abuse.
- 37% of alcohol abusers and 53% of drug abusers also have at least one serious mental illness.
- Among people with lifetime bipolar disorder, around 90% will also have a substance use disorder in their lifetime.
- Among people with lifetime schizophrenia, 47% will have a substance use disorder in their lifetime.
- 25% of people diagnosed with major depression are also diagnosed with a substance use disorder.
These figures underscore that co-occurring disorders are not the exception but often the rule. Recognizing this high prevalence is the first step toward advocating for and implementing integrated care models. For those seeking clarity on their own situation, various tools and assessments are available. Understanding the role of addiction recovery testing can be an important step in accurate diagnosis and tailoring effective treatment. Similarly, specialized dual diagnosis support, such as for individuals navigating dual diagnosis ADHD, acknowledges the unique challenges and pathways to recovery for specific co-occurring conditions.
How Substance Use Impacts Addiction Recovery and Mental Health Outcomes
Substance use and mental health conditions don’t merely exist side-by-side; they actively influence and often exacerbate one another, creating a complex web that can hinder recovery. This intricate interaction is a key reason why integrated treatment is so vital.
One of the most challenging aspects is how substance use can mimic symptoms of mental health disorders. For example, stimulant abuse can induce paranoia and hallucinations, resembling symptoms of psychosis, while alcohol withdrawal can cause severe anxiety and depression. This mimicry makes accurate diagnosis difficult, as clinicians must determine whether symptoms are substance-induced or indicative of a primary mental health condition.
Beyond mimicry, substance use often directly worsens existing mental health conditions. For someone struggling with depression, alcohol might initially provide a temporary lift, but it’s a depressant that ultimately deepens feelings of sadness and hopelessness. Similarly, cannabis use, while sometimes perceived as a way to relax, can intensify anxiety and paranoia, particularly in individuals predisposed to such conditions. These effects lead to a cycle where individuals use substances to cope with worsening mental health, only for the substances to further deteriorate their mental state. The interplay can be particularly devastating for those dealing with the profound effects of dual diagnosis PTSD, where substances might be used to numb traumatic memories, but ultimately prevent true healing.
Substance use can also trigger or intensify anxiety, leading to panic attacks, chronic worry, and social phobias. The physiological effects of many substances, such as increased heart rate and heightened alertness, can directly contribute to anxiety symptoms. Moreover, chronic substance use can alter brain chemistry, making individuals more susceptible to anxiety disorders.
A critical concern in concurrent disorders is medication interference. Many psychotropic medications prescribed for mental health conditions can have dangerous interactions with alcohol or other drugs. Substance use can reduce the effectiveness of these medications, increase their side effects, or even lead to life-threatening complications. This interference undermines the very treatment designed to stabilize mental health, often leading to a frustrating cycle of ineffective care.
These interactions contribute to relapse cycles. When mental health symptoms are poorly managed due to substance use, the risk of returning to substance use increases. Conversely, a relapse in substance use can trigger a severe downturn in mental health, making it harder to maintain sobriety. Breaking these cycles requires comprehensive strategies that address both conditions simultaneously. For those seeking to understand how to break free from this cycle, exploring effective alcoholism treatment programs can provide valuable insights into integrated approaches.

Effective Treatment Approaches for Concurrent Disorders
Treating concurrent disorders effectively requires a specialized and integrated approach that addresses both substance use and mental health conditions simultaneously. Historically, these conditions were often treated separately, leading to fragmented care and poorer outcomes. However, the understanding that these issues are deeply intertwined has paved the way for more holistic and successful treatment models.
The cornerstone of effective treatment for concurrent disorders is integrated care. This model ensures that both mental health and substance use disorders are treated by the same team of professionals, in the same setting, and at the same time. This eliminates the “no wrong door” problem, where individuals might be turned away from mental health services because of their substance use, or from addiction services because of their mental health condition. Integrated care fosters better coordination, reduces the risk of symptoms being overlooked, and improves treatment adherence.
A comprehensive biopsychosocial assessment is the starting point for integrated care. This assessment delves into the biological, psychological, and social factors that contribute to an individual’s condition. It considers genetic predispositions, brain chemistry, thought patterns, emotional regulation, trauma history, family dynamics, social support systems, and environmental stressors. This detailed understanding allows treatment providers to create a truly personalized treatment plan that targets the root causes and maintains the individual’s overall well-being. This personalized approach is often a key feature of inpatient treatment programs, which offer a structured environment for comprehensive care. Many reputable facilities, including those found in regions like California rehab centers, prioritize integrated care for individuals with co-occurring disorders.
Effective integrated treatment often incorporates a range of therapeutic modalities. Below is a comparison of two prominent evidence-based behavioral therapies:
Feature Cognitive Behavioral Therapy (CBT) Dialectical Behavioral Therapy (DBT) Primary Focus Identifying and changing negative thought patterns and behaviors. Teaching emotional regulation, distress tolerance, and interpersonal effectiveness. Key Techniques Cognitive restructuring, behavioral experiments, exposure therapy. Mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness skills. Target Population Wide range of mental health issues, including anxiety, depression, SUDs. Originally for Borderline Personality Disorder, now for various complex issues. Approach Challenges unhelpful thoughts directly. Accepts thoughts/feelings while working to change unhealthy behaviors. Goal Develop healthier coping mechanisms and thought processes. Reduce self-harm, improve relationships, and manage intense emotions. Evidence-Based Behavioral Therapies
Behavioral therapies are cornerstones of effective treatment for concurrent disorders, helping individuals develop healthier coping mechanisms and address underlying psychological issues.
Cognitive Behavioral Therapy (CBT) is widely recognized for its effectiveness. CBT helps individuals identify and challenge negative or distorted thought patterns that contribute to substance use and mental health symptoms. By understanding how thoughts, feelings, and behaviors are interconnected, clients learn to replace unhelpful thoughts with more realistic ones, leading to healthier actions. For example, someone who believes they are a failure might use substances to cope; CBT helps them reframe this thought, reducing the urge to self-medicate.
Dialectical Behavior Therapy (DBT) builds on CBT principles but places greater emphasis on emotional regulation, distress tolerance, and interpersonal effectiveness. DBT is particularly useful for individuals who experience intense emotions, engage in self-harm, or struggle with unstable relationships. It teaches mindfulness techniques to help individuals stay present and aware, and skills to manage overwhelming emotions without resorting to destructive behaviors or substance use.
Motivational Interviewing (MI) is a person-centered counseling style that helps individuals explore and resolve ambivalence about change. Instead of directly confronting resistance, MI gently guides clients to articulate their own reasons for change, fostering intrinsic motivation. This approach is highly effective in encouraging individuals to commit to treatment and recovery goals.
Trauma-informed care is essential for many individuals with concurrent disorders, as trauma often underlies both mental health issues and substance use. This approach recognizes the pervasive impact of trauma and integrates this understanding into all aspects of treatment. It focuses on creating a safe, trustworthy environment and empowering clients to rebuild a sense of control and resilience, rather than inadvertently re-traumatizing them.
Family interventions are also crucial, as addiction and mental health issues affect the entire family system. These interventions involve family members in the treatment process, helping them understand the disorders, improve communication, set healthy boundaries, and develop strategies to support their loved one’s recovery while also addressing their own needs. A holistic approach to healing, which nurtures your journey to wellness through various therapeutic modalities, is vital for long-term success. Resources like those on holistic addiction recovery emphasize the importance of comprehensive care. For a deeper dive into integrated treatment strategies, the Substance Abuse and Mental Health Services Administration (SAMHSA) offers extensive resources on the screening and treatment of co-occurring disorders.
The Role of Medication-Assisted Treatment (MAT)
Medication-Assisted Treatment (MAT) is a highly effective, evidence-based approach that combines medications with counseling and behavioral therapies to treat substance use disorders, particularly opioid use disorder (OUD), and to support mental health. MAT has proven to be a critical component in improving recovery outcomes, reducing relapse rates, and preventing overdose deaths.
For opioid use disorder, specific medications help manage cravings and withdrawal symptoms, allowing individuals to stabilize and engage more fully in therapy. The most common medications used in MAT for OUD include:
- Methadone: A long-acting opioid agonist that reduces cravings and withdrawal symptoms without producing a euphoric high when taken as prescribed. It is typically dispensed in highly regulated clinics.
- Buprenorphine: A partial opioid agonist that also reduces cravings and withdrawal symptoms. It can be prescribed in an outpatient setting by certified doctors, making it more accessible. Often combined with naloxone (Suboxone) to deter misuse.
- Naltrexone: An opioid antagonist that blocks the euphoric effects of opioids. It can be administered daily orally or as a monthly injectable (Vivitrol). Naltrexone is non-addictive and does not cause physical dependence.
These medications for OUD are not simply replacing one addiction with another; they are therapeutic tools that normalize brain chemistry, relieve physiological cravings, and allow individuals to focus on their recovery work. The U.S. Food & Drug Administration (FDA) provides comprehensive information about medications for opioid use disorder, detailing their efficacy and safety.
Beyond OUD, MAT also involves the use of psychopharmaceuticals to treat co-occurring mental health conditions. Antidepressants, anti-anxiety medications, mood stabilizers, and antipsychotics can effectively manage symptoms of depression, anxiety disorders, bipolar disorder, and schizophrenia. When mental health symptoms are stabilized with medication, individuals are better equipped to participate in therapy, develop coping skills, and maintain sobriety.
The integration of MAT into a comprehensive treatment plan, particularly in specialized facilities like those found in Kentucky rehab centers, underscores a commitment to treating the whole person. This combined approach addresses both the physiological and psychological aspects of concurrent disorders, paving the way for more stable and sustained recovery.
Practical Strategies for Long-Term Wellness and Relapse Prevention
Achieving initial sobriety or mental health stability is a significant accomplishment, but sustainable recovery is a lifelong journey that requires ongoing effort and the development of practical strategies. These strategies empower individuals to manage challenges, maintain well-being, and prevent relapse.
A crucial first step in this ongoing process is regular self-assessment. This involves checking in with oneself to monitor mood, energy levels, cravings, and overall mental state. Recognizing early warning signs of distress or potential triggers allows for proactive intervention. This self-awareness is foundational to effective stress management. Chronic stress is a common trigger for both substance use and mental health setbacks. Learning healthy ways to cope with stress—such as mindfulness, deep breathing exercises, progressive muscle relaxation, or engaging in hobbies—is vital.
Cultivating a healthy lifestyle forms the backbone of long-term wellness. This includes prioritizing adequate sleep, maintaining a balanced diet, and incorporating regular physical activity. Exercise, in particular, is a powerful mood booster and stress reducer, contributing significantly to both physical and mental health. Engaging in practices like those found in a yoga for recovery guide can offer a path to integrating physical movement with mental calm.
Here is a list of healthy coping mechanisms that can be integrated into daily life:
- Mindfulness and Meditation: Practicing present-moment awareness to observe thoughts and feelings without judgment.
- Regular Exercise: Engaging in physical activity to boost mood, reduce stress, and improve sleep.
- Creative Expression: Pursuing hobbies like art, music, writing, or crafting as an outlet for emotions.
- Journaling: Writing down thoughts and feelings to process experiences and gain perspective.
- Connecting with Nature: Spending time outdoors to reduce stress and improve mood.
- Healthy Boundaries: Learning to say no and protect one’s time and energy.
- Seeking Support: Reaching out to trusted friends, family, or support groups.
- Problem-Solving Skills: Developing practical approaches to address life’s challenges.
- Relaxation Techniques: Practicing deep breathing, progressive muscle relaxation, or guided imagery.
- Engaging in Meaningful Activities: Pursuing passions and activities that bring joy and purpose.
For ongoing support and connection, especially in today’s digital age, participating in virtual recovery meetings can provide accessible and consistent peer support, reinforcing these healthy coping strategies.
Navigating Post-Pandemic Recovery Challenges
The COVID-19 pandemic introduced unprecedented challenges to mental health and addiction recovery, exacerbating existing vulnerabilities and creating new obstacles. The widespread experience of social isolation due to lockdowns and social distancing measures significantly impacted individuals in recovery. Isolation can breed loneliness, depression, and anxiety, which are potent triggers for relapse. Many support group meetings moved online, which, while offering accessibility, sometimes lacked the immediate, in-person connection crucial for some individuals.
The uncertainty, fear, and grief associated with the pandemic also placed immense strain on mental well-being globally. For those already managing concurrent disorders, these added stressors often led to increased substance use or a worsening of mental health symptoms. It became more difficult to access in-person therapy, medical appointments, and other essential support services, creating gaps in care.
In response to these challenges, building resilience became more critical than ever. Individuals and communities adapted by leveraging technology for virtual support, focusing on self-care, and finding new ways to connect. Resources like the Mental Health during COVID-19 Fact Sheet and guides on coping with self-isolation proved invaluable, offering practical advice and strategies to navigate the unique psychological impacts of the pandemic. Integrating lessons learned from this period, particularly around digital support and flexible care models, will be essential for strengthening recovery pathways.
Building a Supportive Environment and Aftercare
A crucial component of sustainable recovery is establishing a robust, supportive environment and engaging in comprehensive aftercare. Recovery doesn’t end when formal treatment concludes; it’s a continuous process that benefits immensely from ongoing support and strategic planning.
Aftercare, also known as continuing care, is designed to reduce relapse rates and help individuals maintain sobriety and mental well-being long-term. A personalized aftercare plan, developed with a care team, outlines specific treatment options, support groups, and lifestyle habits to follow post-residential care. This plan is dynamic, adapting as an individual’s needs evolve.
Key elements of a supportive environment and aftercare include:
- Sober Living Environments: These structured, drug- and alcohol-free residences provide a safe and supportive transition from inpatient treatment back into independent living. They offer accountability, peer support, and a stable foundation for practicing recovery skills.
- Peer Support Groups: Programs like SMART Recovery and Alcoholics Anonymous provide invaluable peer support. These groups offer a sense of community, shared experience, and mutual encouragement, reminding individuals that they are not alone in their journey. Peer support is highly effective in maintaining motivation and providing practical advice from those with lived experience.
- Alumni Programs: Many treatment centers offer alumni programs that help former clients stay connected with the facility and with each other. These programs often include regular meetings, social events, and opportunities to mentor newer individuals in recovery, fostering a strong, ongoing community.
- Ongoing Therapy and Counseling: Continuing individual or group therapy sessions after intensive treatment helps reinforce coping mechanisms, address new challenges, and process deeper emotional issues.
- Personalized Treatment Plans: As recovery progresses, an individual’s specific needs may change. Regularly revisiting and adjusting personalized treatment plans ensures that the support system remains relevant and effective.
Building a supportive environment also means consciously surrounding oneself with positive influences, setting healthy boundaries with unsupportive individuals, and communicating openly with trusted friends and family about recovery needs. This network acts as a buffer against stressors and a source of encouragement, significantly enhancing the chances of sustained recovery.
Supporting Loved Ones and Reducing Social Stigma
The journey of addiction and mental health recovery is rarely traveled alone. Family and friends play a crucial role, but they also need guidance on how to provide effective support while maintaining their own well-being. Furthermore, societal stigma remains a significant barrier to seeking help and achieving lasting recovery, underscoring the need to reduce it.
For family and friends, offering family support means understanding that addiction and mental health disorders are complex health conditions, not moral failings. Education about concurrent disorders can help loved ones navigate the challenges with empathy and patience. This involves learning about the nature of the conditions, the treatment process, and the potential for relapse.
However, support must be balanced with the establishment of healthy boundaries. This protects both the individual in recovery and their loved ones from enabling behaviors or burnout. Boundaries might involve not providing financial support for substance use, refusing to tolerate abusive behavior, or ensuring that consequences for actions are upheld. A brochure on supporting a loved one (even if focused on cancer, the principles of support are transferable) can offer valuable insights into caregiving while maintaining personal well-being.
Crucially, stigma-reducing language is paramount when discussing addiction and mental health. The words we use shape perceptions, and traditional language often perpetuates negative stereotypes, shame, and discrimination. Adopting person-first language is a key practice:
- Instead of “addict,” say “person with a substance use disorder.”
- Instead of “mentally ill,” say “person experiencing a mental health condition.”
- Instead of “clean” or “dirty,” say “in recovery” or “using substances.”
This shift in language emphasizes the individual’s humanity over their condition, fostering respect and encouraging help-seeking behavior. Organizations like Shatterproof provide excellent resources on stigma-reducing language, advocating for a vocabulary that promotes understanding and compassion. By actively using person-first language and challenging stigmatizing narratives, we contribute to a more supportive environment where individuals feel safe to seek and embrace recovery.
Resources and Support Systems in New Brunswick and Beyond
Access to comprehensive and timely support is critical for individuals navigating addiction and mental health recovery. In New Brunswick, Canada, and across national landscapes, a variety of resources are available to assist individuals and their families.
Horizon Health Network plays a significant role in New Brunswick, offering a wide range of services for substance misuse, harmful gambling, and mental health issues across all age groups. Their programs include individual and group counseling, detoxification services, opioid replacement therapy, and short- and long-term rehabilitation. Horizon’s commitment extends to providing accessible, community-based crisis response.
For immediate crises, several helplines and services are available:
- Mobile Crisis Units: These teams provide timely interventions in community settings, often available evenings and weekends, responding to individuals and families in their chosen environment. They help de-escalate situations and connect individuals to appropriate care.
- 9-8-8 Suicide Crisis Helpline: A national, toll-free, 24/7 service for anyone thinking about suicide or worried about someone they know. This vital resource offers immediate support and connection to mental health professionals.
- Tele-Care 811: This 24/7 service provides free, confidential health advice from a registered nurse. It’s an excellent first point of contact for health concerns, including mental health, and can guide individuals to appropriate services. You can learn more about Tele-Care 811 for immediate health guidance.
- Bridge the gap: An invaluable online resource designed to support mental wellness, offering tailored information and tools for both youth and adults. For adults seeking mental health support, Bridge the Gap Adult provides comprehensive resources.
- Chimo Helpline: A New Brunswick-based crisis line providing confidential and anonymous support 24/7. The Chimo Helpline is a vital local resource for those in distress.
- New Brunswick 211 Services: For a comprehensive directory of community and social services, Find Help: New Brunswick 211 Services is an excellent resource that connects individuals to local support for everything from housing to mental health.
These resources, both regional and national, form a critical safety net and pathway to recovery. They emphasize that help is available, often just a phone call or click away, and that no one needs to face their challenges alone.
Frequently Asked Questions about Addiction and Mental Health
Navigating addiction recovery and mental health can bring many questions. Here, we address some of the most common inquiries to provide clarity and guidance.
What are the primary signs of a co-occurring disorder?
Recognizing the signs of a co-occurring disorder, or dual diagnosis, is the first step toward seeking appropriate help. These signs often involve a complex interplay between substance use and mental health symptoms, making them sometimes difficult to distinguish. Key indicators include:
- Sudden Mood Swings: Experiencing rapid and intense shifts in mood, from euphoria to deep despair, often seemingly without external cause.
- Using Substances to Cope with Emotions: Regularly turning to alcohol or drugs to manage feelings of anxiety, depression, stress, or trauma.
- Withdrawal from Social Activities: Losing interest in hobbies, friends, and family activities that were once enjoyed, preferring isolation.
- Increased Tolerance and Dependence: Needing more of a substance to achieve the desired effect, or experiencing withdrawal symptoms when not using.
- Neglecting Responsibilities: Failing to meet obligations at work, school, or home due to substance use or mental health struggles.
- Persistent Feelings of Hopelessness or Anxiety: Chronic feelings of sadness, worry, fear, or an inability to experience pleasure, which may be exacerbated by substance use.
If you or someone you know exhibits these signs, it’s important to seek a comprehensive assessment to determine whether concurrent disorders are present. For guidance on where to find such services, exploring comprehensive addiction services can be a valuable starting point.
How can I access immediate crisis support in New Brunswick?
For immediate crisis support in New Brunswick, several vital resources are available 24/7:
- Call 911: For any life-threatening emergency, including immediate danger to oneself or others.
- Dial 811 (Tele-Care): For confidential health advice from a registered nurse, including mental health concerns, and guidance on accessing local services.
- Contact the Chimo Helpline: Call 1-800-667-5005 for confidential, anonymous crisis support.
- Use the 9-8-8 Suicide Crisis Helpline: This national, toll-free, 24/7 service at 9-8-8 is available for anyone thinking about suicide or worried about someone they know.
- Text 45645: For text-based crisis support from Talk Suicide Canada between 5 p.m. and 1 a.m. EST. More information can be found at Talk Suicide Canada.
These resources are designed to provide immediate assistance and connect individuals to the help they need during times of acute distress.
What is the success rate for recovery from concurrent disorders?
Defining “success” in recovery can be complex, as it often refers to a spectrum of outcomes, from sustained abstinence to significant improvements in mental health and overall quality of life. However, data indicate that recovery from concurrent disorders is not only possible but also achievable for a large number of individuals.
As noted earlier, a significant 72.1% of U.S. adults who perceived they had ever had a substance use and/or mental health problem considered themselves to be in recovery or recovered. This statistic highlights the immense capacity for healing and personal growth.
Key factors influencing these positive outcomes include:
- Integrated Treatment: Studies consistently show that integrated treatment, which addresses both mental health and substance use disorders concurrently, leads to significantly better outcomes compared to treating the conditions separately.
- Long-Term Support: The availability of ongoing support, including aftercare programs, peer support groups, and continued therapy, is crucial for reducing relapse rates and sustaining recovery over time.
- Personalized Care: Treatment plans tailored to an individual’s specific needs, incorporating their unique challenges, strengths, and goals, enhance engagement and effectiveness.
While recovery is often a non-linear process with potential setbacks, the overall picture is one of hope and progress. The Substance Abuse and Mental Health Services Administration (SAMHSA) regularly publishes reports on recovery, such as the Recovery from Substance Use and Mental Health Problems Report, which provides valuable insights into national recovery trends and factors. These resources underscore that with the right support and commitment, a fulfilling life in recovery is well within reach.
Conclusion
The journey through addiction recovery and mental health challenges is profound, marked by resilience, growth, and the unwavering pursuit of well-being. We have explored the intricate connections between substance use and mental health, the prevalence of co-occurring disorders, and the critical importance of integrated treatment approaches. From evidence-based therapies like CBT and DBT to the vital role of Medication-Assisted Treatment, the pathways to healing are diverse and effective.
Sustainable recovery is not a destination but a continuous process, nurtured by practical wellness strategies, strong support systems, and a commitment to reducing social stigma. The availability of resources, both local and national, underscores that help is always within reach, offering hope and guidance through every step.
This journey demands persistence, courage, and the understanding that setbacks are part of the process, not a sign of failure. By embracing integrated care, fostering supportive environments, and advocating for compassionate language, we can collectively build a society that empowers individuals to achieve their fullest potential.
If you or a loved one is ready to take the next step on this transformative journey, support is available. SoberSteps personalized addiction mental health plans can help you explore integrated care options and next steps toward recovery. To learn more about our philosophy and commitment to integrated care, please visit our About SoberSteps page. Together, we can navigate these pathways to sustainable recovery.